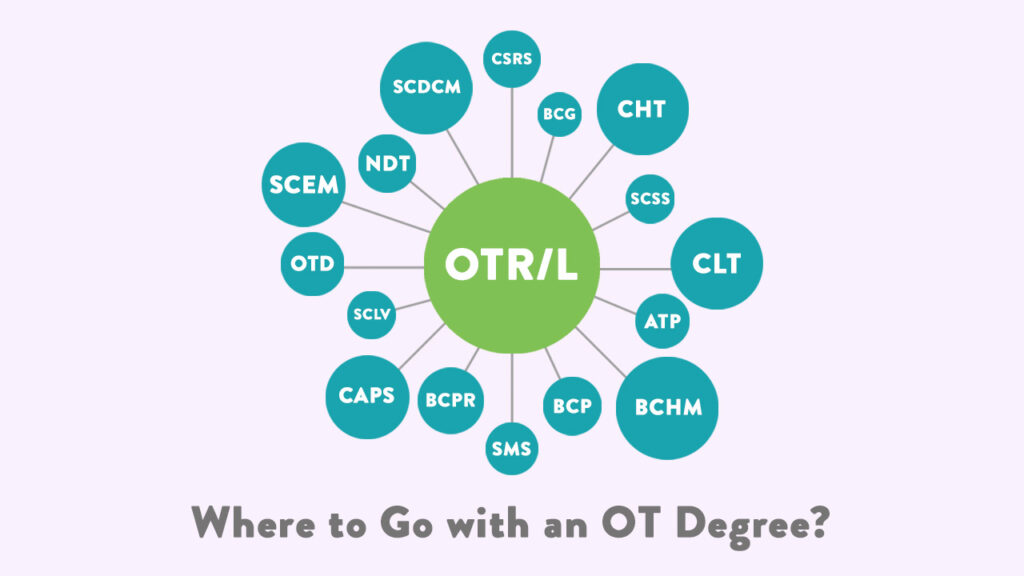
Occupational therapy, physical therapy, and speech therapy are often collectively referred to as the “rehabilitation therapy team.”
But wait—what, exactly, is the rehabilitation therapy team?
We’re so glad you asked!
In fact, there are so many questions around what rehabilitation is, and who does what within the rehab world, that I teamed up with Amy Behrens, CCC-SLP and Meredith Castin, PT, DPT to write this article.
We think it’s time to create a single resource that says exactly what we do.



As firm believers that medicine works best with a collaborative approach, we want to not only help people understand what physical therapy (PT), occupational therapy (OT), and speech-language pathology (SLP) are, but also how they are similar and different.
Our goals for writing this article are to help the medical community better understand our roles, ensure that patients know how we bring our unique training and skills to help them recover—and hopefully to help future rehab professionals discover which therapy path they wish to pursue, should they decide to join our ranks!
Without further ado, let’s dive in!

What is rehabilitation therapy?
Rehabilitation therapy refers to evaluations, interventions, and treatments that help patients regain function.
A rehabilitation therapy team comprises physical therapy, occupational therapy, and speech-language pathology professionals, all of whom work together to provide care to patients whose lives have been affected by disease, injury, or disability.
As a team, therapists help to address impairments in patients’ ability to move, speak, eat, walk, dress themselves, and otherwise participate in their normal daily lives.
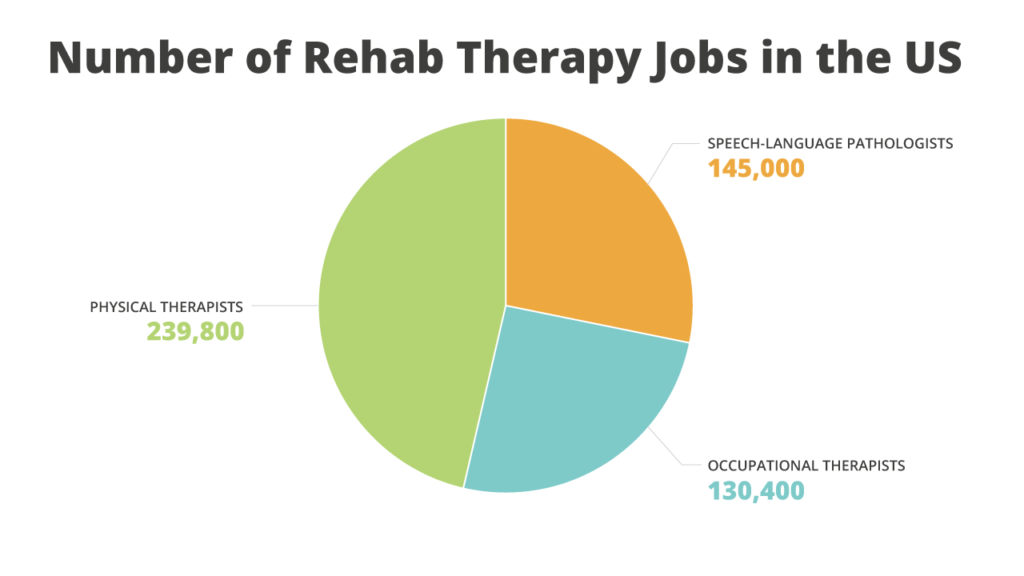
According to the US Bureau of Labor Statistics, there are 145,100 SLP jobs, 130,400 OT jobs, and 239,800 PT jobs in the US.

What is occupational therapy (OT)?
Being that this is an occupational therapy site, let’s start there. What, exactly, is occupational therapy?
The short version is that OTs are health professionals who work with people who’ve had illnesses, injuries, and disabilities that prevent them from participating in their normal daily activities.
OTs work with these individuals to help them regain agency over their own health in various ways, including helping them with cooking, bathing, dressing, toileting, and more. In some cases, that involves using assistive technology, or it might require providing splinting, bracing, or other devices.
Because OT is a very holistic profession, we approach each task with the big picture of the patient’s life in mind.
That’s the short version of what we do! I created a whole article called “What is Occupational Therapy & How Can It Help You?”—and you can read that if you want the long version.

What is physical therapy (PT)?
Simply put, physical therapy is the treatment of the effects of disease, injury, and disability by using exercise, manual therapy, education, and therapeutic activity. PTs are considered a conservative care option because they use such techniques to get results, rather than relying on medications or surgery.
Physical therapists’ primary goals are to help patients improve their movement and function, and also reduce their pain. Physical therapists often prescribe stretches, exercises, and functional mobility activities to help patients move more efficiently and effectively, while eliminating as much pain as possible.
Physical therapists also look at patients from a holistic lens, but they are generally focused more on providing specific interventions to improve particular movements.

What is speech-language pathology (SLP)?
A speech-language pathologist’s goal is to improve a patient’s ability to communicate and/or swallow. SLPs can work on many aspects of communication with patients, including speech production, fluency (stuttering), language, cognition, voice, resonance, and hearing. Swallowing evaluation and treatment can also include feeding.
SLPs work with individuals across the life span, and with a variety of diagnoses (ranging from stroke to autism spectrum disorder to head and neck cancer to traumatic brain injury to vocal fold nodules!). The services provided by SLPs can be either rehabilitative (helping patients to regain what they have lost) or habilitative (helping patients to maintain or improve communication and/or swallowing ability).
SLPs also strive to look at a patient and his or her goals in a holistic manner. Communicating effectively and swallowing safely can play a huge role in a patient’s ability to participate in social rituals like mealtime, to make their wants and needs known, to connect with their loved ones, or to continue working in a specific vocation. SLPs work with patients and their families on individualized goals that they develop based on each patient’s unique situation, and what will improve that patient’s quality of life.
For more reading on speech-language pathology, here is their scope of practice.
OT vs. PT. vs. SLP: similarities and differences
As noted earlier, physical, occupational, and speech therapy are all primarily concerned with improving patients’ function.
It’s how we each evaluate and treat a patient that sets us apart.
We’ll get into that in a moment, but let’s start with some similarities.
Similarities
Here are some ways that the rehab therapy team’s roles overlap a bit.
- We all follow a similar trajectory of treatments: initial evaluations, progress notes, and discharges.
- We all focus on caregiver training to help support a patient with the end goals.
- We all often provide somewhat similar treatments (as noted above) and work toward similar end goals––though each in our own unique manners.
- We all generally work in similar settings. For example, you’ll find all three of us in acute care, LTAC, inpatient rehab, SNF, pediatric, school, home health, and outpatient settings.
- We are all key in making discharge recommendations after patients are hospitalized.
- We all participate in research and education.
- We all share some similar areas of focus, such as working with children or older adults. PTs and OTs share some subspecialties and niches, such as hand therapy and pelvic health––and OTs and SLPs both work on cognitive and mental health interventions, especially with patients who have dementia or have experienced brain injuries/diseases.
Differences
Here are some of the ways that each rehabilitation therapy profession is unique.
OTs are unique because they use a holistic lens to focus on daily tasks. From driving to dressing oneself, an OT can help people become as involved as possible in the activities they love…sometimes getting quite creative with splinting or assistive technology in the process! Plus, OTs can pursue a niche in mental health!
SLPs are unique because they focus on the incredibly important functions of swallowing and communication. From performing instrumental evaluations for voice and swallowing to using AAC (augmentative and alternative communication) technology to help patients communicate, SLPs have limitless niches and specializations. Some SLPs even focus on transgender communication or literacy!
PTs are unique in that they can work with professional athletes, sports teams, dance troupes, or other movement-based groups of people. They can also pursue pain science, and even work with horses, dogs, and cats in the field of animal rehabilitation!
Our teamwork approach in action.
Perhaps the best way to explain the similarities and differences in the rehab therapies is to use a patient case study as an example.
Let’s consider the case of a young man who has chronic high blood pressure and then has a cerebrovascular accident (CVA), which is commonly referred to as a stroke. A stroke is sometimes informally called a “brain attack” because it involves the sudden deprivation of oxygen to the brain. This leads to areas of the brain either temporarily or permanently losing function.
So, let’s look at how each therapy discipline will treat the man who has a stroke.
An occupational therapist focuses primarily on how this patient (whom an OT will often refer to as a client) is able to function in his daily roles, based on the damage to various parts of his brain.
- Can this man cook meals for his young daughter?
- If not, an OT will provide coaching, exercises, and adaptive equipment to help the man return to cooking the meals he and his family love.
A physical therapist also looks at that same young man and wonders how he is functioning from a movement standpoint.
- Can the patient safely walk 50 feet so he can care for his daughter while his wife is at work?
- If not, a PT will provide exercises, assistive device (cane, walker, etc.) training, and manual therapy to help the patient regain the ability to walk as independently as possible.
As you can see, there is already some overlap in function. After all, that patient or client will need to walk to and from the pantry to get the supplies for cooking, too!
If the patient needs to stand up independently to cook, he will need strength and balance in his legs. That means both OTs and PTs might be working on similar goals of standing tolerance, which will help him be able to be more independent. But the PT looks at walking independently as the end goal, while the OT looks at cooking meals as part of a normal daily life as the end goal.
A speech-language pathologist also looks at this same patient from a functional standpoint, with the emphasis being on communication and swallowing. In addition, the SLP will consider the patient’s cognition. In fact, there’s a big overlap between SLPs and OTs, especially in settings like acute care, inpatient rehab, and outpatient.
- Can the patient speak to his wife without struggling to find the right words (this is called aphasia)? And can this patient move his mouth, jaw, and tongue to speak without struggling to articulate (this is called dysarthria)?
- If not, the SLP might work with this patient to improve his ability to communicate so that his wife can purchase the foods that he wants for dinner.
Differences in education
PTs and OTs have very similar curriculums in some ways, which is why some schools even have us sitting in the same rooms for a few courses!
SLP’s curriculum is probably the most different from the rest, but we do all share some core commonalities.
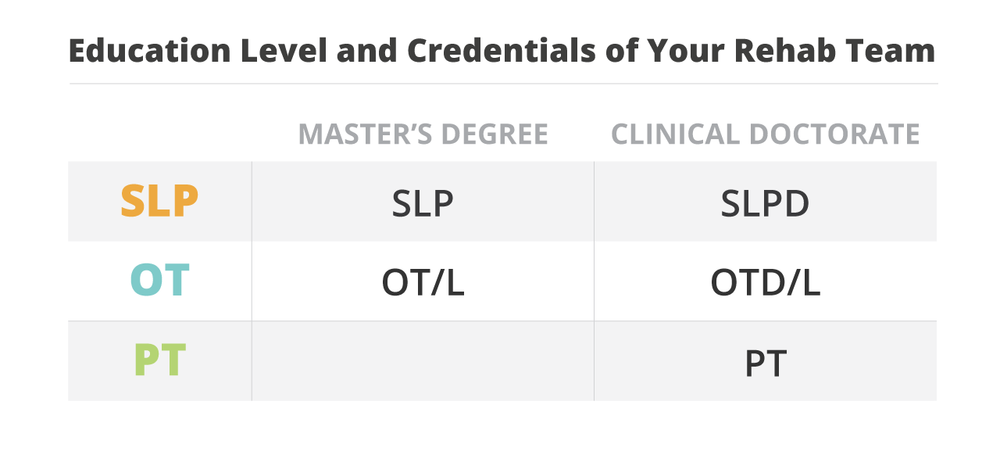
Before we jump into the coursework itself, keep in mind that occupational therapists and speech-language pathologists need master’s degrees to practice, while the entry-level requirement for physical therapists is a doctorate degree. WebPT has a comprehensive article about all the nuances of becoming a PT. And, we’ve recently put together a post that walks you through what it takes to become an OT.
All three disciplines have coursework in human anatomy, physiology, and neuroscience. Occupational and physical therapists both have additional focus on orthopedics, neurological interventions, geriatrics and pediatrics. OTs branch off to focus on activity analysis, cognitive function, mental health, and research. PTs spend extended amounts of time on joint mobilization, therapeutic exercise, and pain science, as well as the pulmonary, digestive, integumentary (skin), and other body systems that impact movement.
Speech-language pathologists spend a good part of their curriculum studying speech, language, and voice disorders, and also focus on specific speech and swallowing disorders that affect both children and adults.
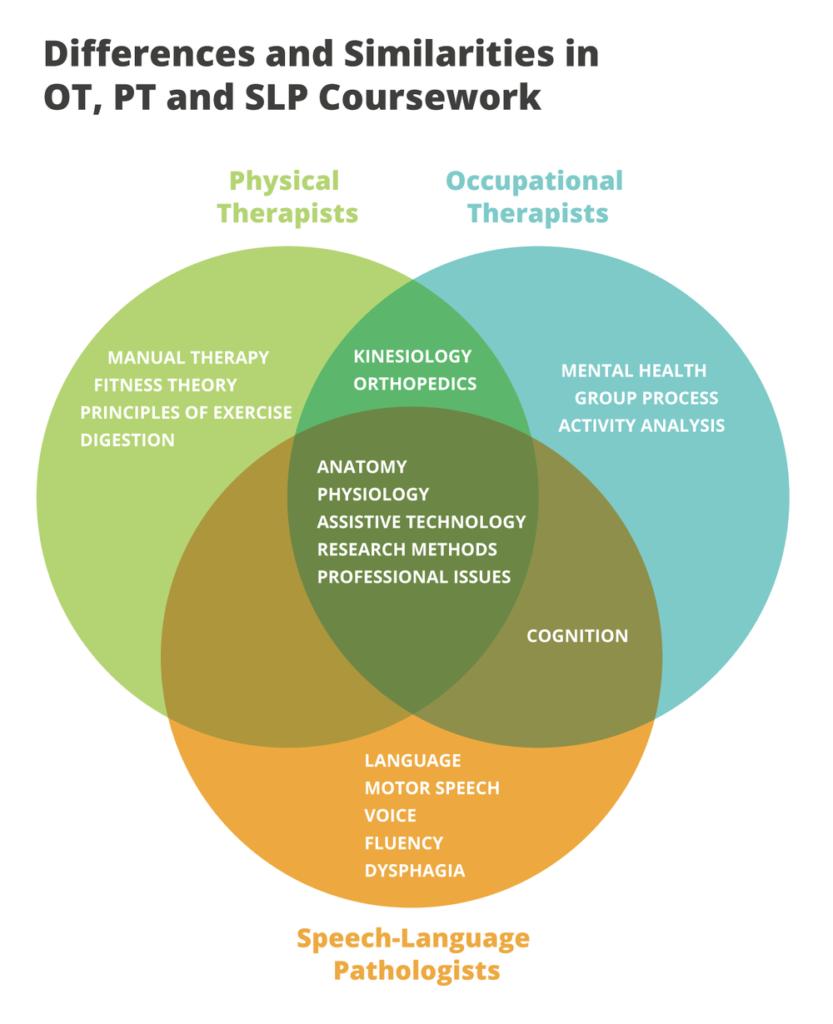
If you’d like to take a deeper dive into each profession’s focus, check out each program’s curriculum at NYU!
Differences in licensure
All new physical therapy students in the U.S. must complete a Doctor of Physical Therapy (DPT) degree at one of the accredited institutions across the US. In order to practice, they must also pass the NPTE (National Physical Therapy Exam) and apply for and receive a state license.
In order to become educated as an occupational therapist in the US, one must obtain a master’s degree from an accredited OT school, then pass the NBCOT (National Board for Certification of Occupational Therapists).
In the US, speech-language pathologists must complete a master’s degree-level program, pass a Praxis exam, and obtain licensure through individual states in order to practice.
Many speech-language pathology positions also require SLPs to have earned (or be working toward earning) their Certificate of Clinical Competence (CCC) through the American Speech-Language-Hearing Association (ASHA). This certification requires the SLP complete a clinical fellowship year (among other requirements).
Each state has different requirements for PTs, OTs, and SLPs to obtain and maintain licensure, so therapists must consider individual state laws, regardless of whether they have been educated on US soil or elsewhere.
OT vs. PT vs. SLP salary
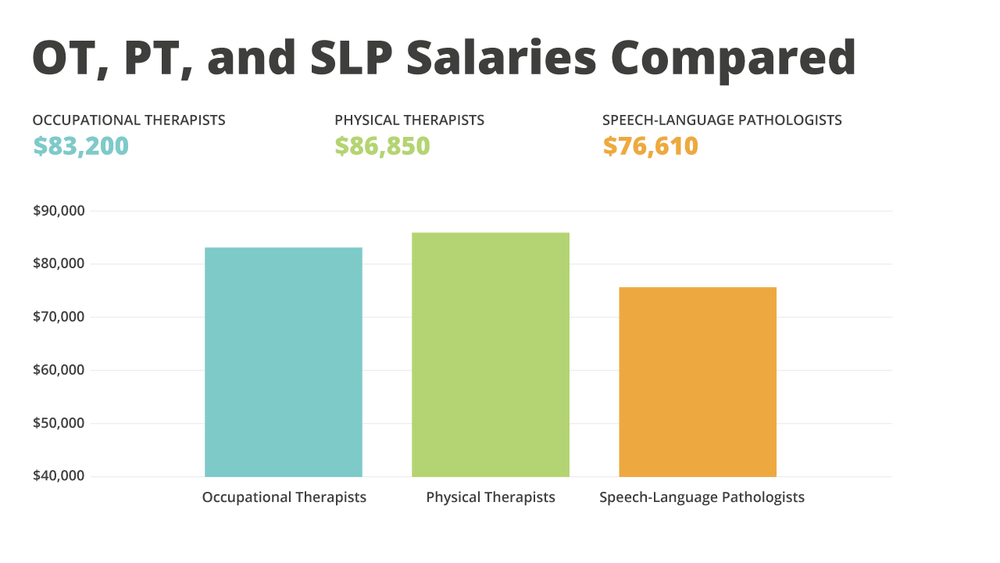
According to the Bureau of Labor Statistics, PTs, OTs, and SLPs have somewhat similar salaries.
The largest gap seems to be between PT and SLP.
The BLS site reports that the median annual wage for physical therapists was $86,850 in May 2017, and it was $76,610 for Speech-Language Pathologists. The median wage for OTs fell squarely in the middle of that range, at $83,200.
As this is an OT website, we have our own guide to OT salary, in case you want to dive deeper into that particular data.
Keep in mind that median wage is the pay at which half the workers in an occupation earn more than that pay, and half earn less.
Another thing to keep in mind is saturation. Certain cities will have several PT, OT, or SLP schools within the area (or at least nearby), so there is more competition for jobs, lowering overall wages.
Also, more “desirable” cities will often pay lower rates because more people are vying for the jobs there.
Aside from location, the setting in which you practice—as well as your employer—will play a big role in how much you earn.
Our advice is to consider the field that appeals the most to you, rather than looking at the salary alone, to ultimately make your decision.
OT vs. PT vs. SLP debt reduction
As mentioned earlier, all three disciplines require a post-baccalaureate degree to practice. OTs and SLPs need master’s degrees, while PTs need doctorates.
Master’s degrees and doctorates are usually not cheap, so it’s important to realize that most people who become rehab therapists do incur significant debt in the process.
While there have been a number of articles addressing the problem in the physical therapy field, there isn’t as much chatter about OT and SLP. This might be because the burden of debt from a master’s degree is less than that of a doctorate.

Our advice is to consider your own debt burden based on how your life will be impacted by the cost of school. Based on your current financial situation, needs of dependents or family members, spending habits, and other factors, you may or may not find that becoming a therapist is financially feasible for you.
While some schools do carry more clout than others, where you attend school does not typically affect your pay upon hire, so we recommend you choose the least expensive option (considering room and board and other living expenses) for school.
Overall, as wonderful as the rehab therapy professions are, the the debt to income ratio can be hard to bear.
At the end of the day, we encourage anyone to do a LOT of shadowing in their profession of choice before signing up for a heavy debt load!
Common practice niches and settings
One of the best things about being a therapist is the ability to explore all sorts of settings and patient populations, and to delve deeper and expand your expertise in the areas that interest you most!
PTs, OTs, and SLPs can all choose to focus on infants, children or adults, and each can choose whether to practice primarily in an inpatient or outpatient setting. OTs, PTs, and SLPs can also opt to work in the school system.
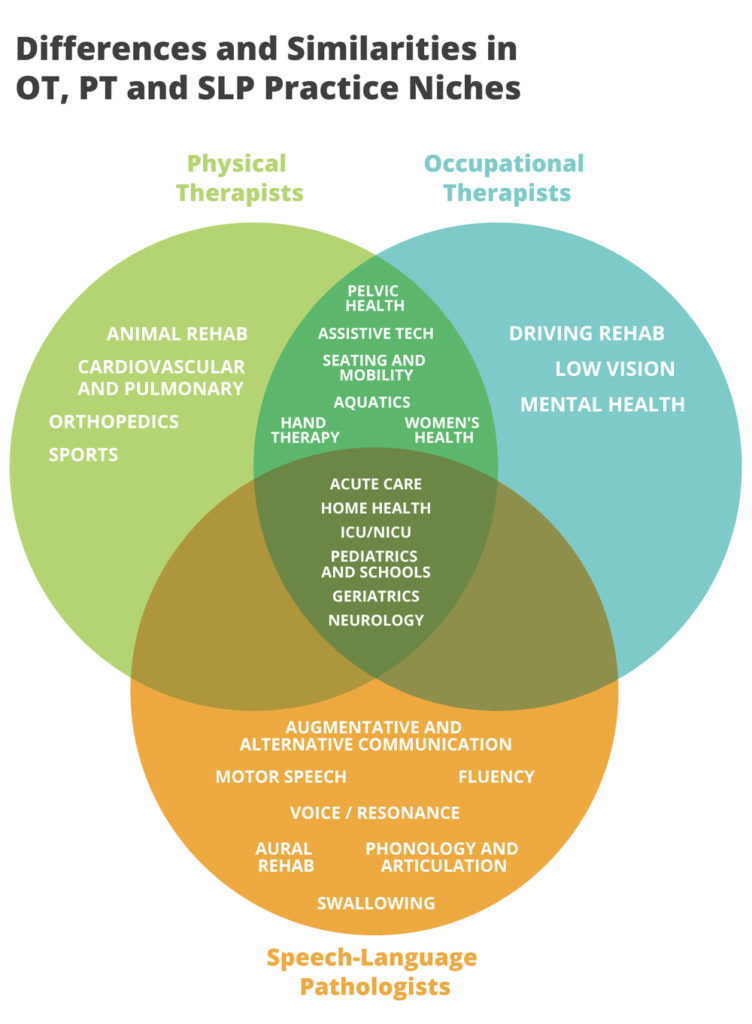
Physical therapists commonly choose niches such as geriatrics, pediatrics, hand therapy, sports, and pelvic health. A newer one is animal therapy, particularly with dogs. More and more PTs are entering the realm of pain science these days, too, which is great considering the opioid crisis in the US!
Occupational therapists often opt for specialized training in driving rehab, low vision, hand therapy, and mental health.
Speech-language pathologists frequently choose to focus on fluency, swallowing disorders, and voice/resonance disorders.
Industry trends for rehab therapists
Despite the differences in specializations and niches, there are several industry trends that are gaining popularity across the three rehab fields.
Here are some of them:
Non-traditional and non-clinical careers
More and more PTs, OTs, and SLPs are opting to leverage their degrees in alternative settings, outside of traditional, direct patient care. There are many reasons for this, including boredom, glass ceilings, and burnout—but many people choose to go non-clinical simply because they’re ready to try something new and use their degrees and education in creative ways.
Meredith and I wrote an article about non-traditional options for occupational therapists, and she runs an entire website around non-clinical jobs for rehab professionals! Some of her offerings include courses, articles, videos, interviews, and career coaching—all of which focus on helping PTs, OTs, and SLPs find non-clinical ways to use their degrees.
Telehealth
Teletherapy is all the rage these days. Initially, SLPs were the first to get on board with treating remotely, but now more and more OTs and PTs are joining the ranks of online therapists. There are many ways to get involved, and you can read my article about telehealth OT and Meredith’s article about telehealth PT for more information.
Travel
The demand for therapists is higher than ever, and some facilities have a difficult time meeting staffing needs. Whether these facilities are in remote or “undesirable” locations, or they simply don’t have any nearby grad schools, they will often opt to hire travelers to fill short-term staffing needs.
Traveling can be great for new and experienced therapists alike. In addition to paying significantly more than pretty much any normal full-time job (with very few exceptions), travel offers a unique opportunity to work with a wide variety of patient populations in various settings, all in a very short time period. Plus, travel therapy is a great way to see the country!
OT vs. PT vs. SLP job outlook
According to the Bureau of Labor Statistics (BLS), all three rehab therapy professions have an excellent employment outlook.
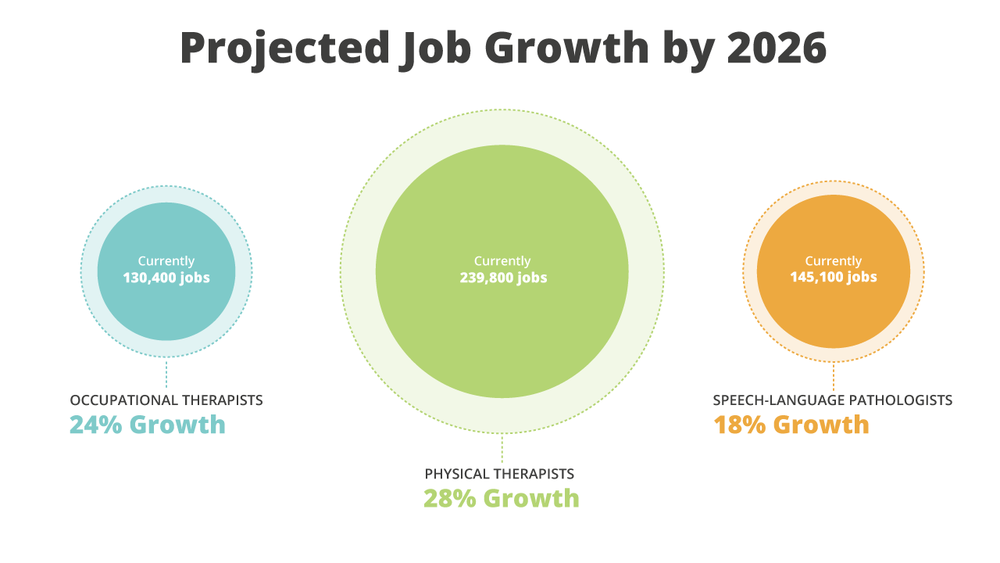
Employment of occupational therapists is projected to grow 24 percent from 2016 to 2026, which is much faster than the average for all occupations. Occupational therapy will continue to be an important part of treatment for people with various illnesses and disabilities, such as Alzheimer’s disease, cerebral palsy, autism, or the loss of a limb.
Employment of physical therapists is projected to grow 28 percent from 2016 to 2026, which is also much faster than the average for all occupations. Demand for physical therapy will come from the aging baby boomers, who are not only staying active later in life, but are also more susceptible to age-related health conditions that may require physical therapy. In addition, physical therapists will be needed to treat people with mobility issues stemming from chronic conditions, such as diabetes or obesity.
Employment of SLPs is projected to grow 18 percent between 2016 to 2026, With baby boomers continuing to age, there will be increased need for SLPs to treat speech and language impairments caused by strokes and age-related brain injuries.
The history of OT, PT, and SLP
We thought a brief overview of our professions’ histories was important to include, because it emphasizes two things:
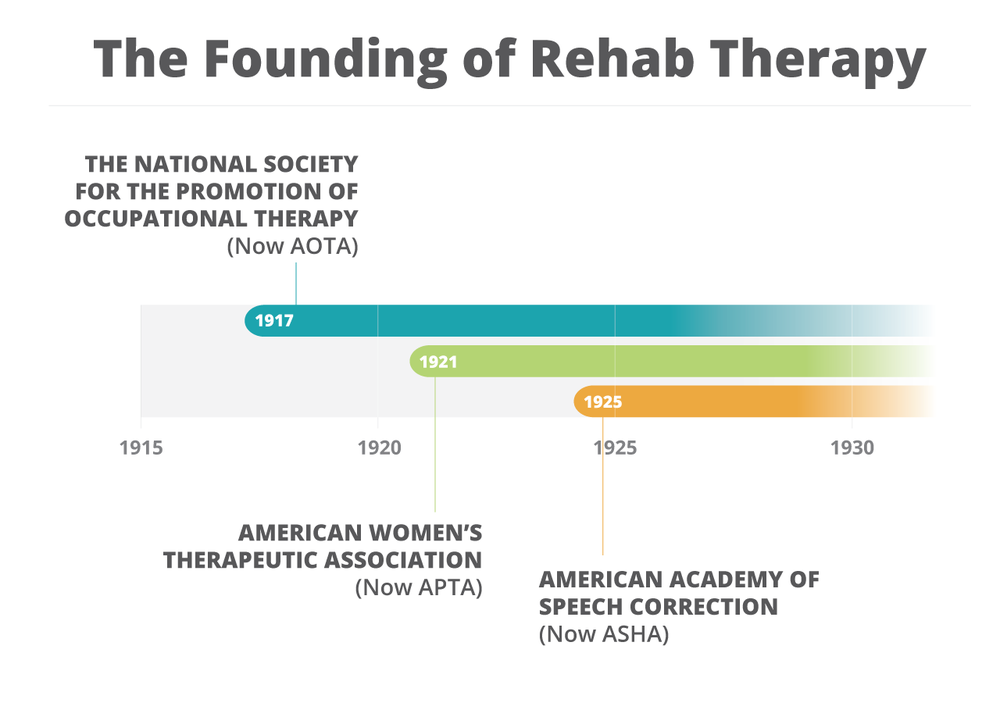
- All three professions are around a century old, making them relatively new
- Though distinct in their own ways, our professions have much commonality in their history
All three professions were started around the same time and two major factors influenced their founding:
- World War I
- The entrance of women into the workforce
We look forward to seeing how all three grow evolve and continue to interact with one another.
No matter which path you choose, you’re in good shape.
The rehab therapy professions are constantly making various lists of the top careers in America.
And while these lists should always be taken with a grain of salt, it’s always nice to see our wonderful professions represented positively by mainstream media!
Here are just a few of our bragging rights:
- Glassdoor’s 2018’s 50 Best Jobs in America (OT #4, SLP #35)
- US News and World Report’s 25 Best Healthcare Jobs (OT #9, PT #10, SLP #24)
- Money Magazine’s 100 Best Jobs (OT # 11, PT #12, SLP #38)
We are all one big, happy rehab family!
At the end of the day, our differences and similarities are what make us such a fantastic team.
One of the reasons we love each other so much is that we understand the joys and pains involved with rehabilitating patients to achieve their goals.
We hope that this article has helped un-muddy the waters by clarifying what the rehabilitation therapy disciplines do, and also how we work together and separately to help patients regain the ability to communicate, eat, move, and participate in the activities that mean the most to them.
And if you’re trying to decide which path to pursue, we hope this article has helped you make that choice!
About the authors:
Meredith Castin, PT, DPT is a physical therapist based in San Diego who worked in outpatient, acute care, inpatient, and pretty much every other setting out there, before ultimately leaving patient care to become a writer. In addition to writing as a freelancer for OT Potential and WebPT, Meredith runs The Non-Clinical PT, an educational platform devoted to helping rehabilitation therapy professionals leverage their degrees and experience in non-clinical careers.
Amy Behrens, MA, CCC-SLP is a speech language pathologist whose work gives her the opportunity to work with adults and children in the outpatient, inpatient, and acute care settings. When she’s not helping folks to communicate or swallow, she loves exploring the Minnesota Northwoods (ideally by canoe!).
Sarah Lyon, OTR/L is and occupational therapist, and is the owner of OT Potential. Sarah worked in an acute trauma center, a rural hospital, and a state psychiatric hospital before transitioning to helping fellow OTs full-time—by creating resources such as this one.